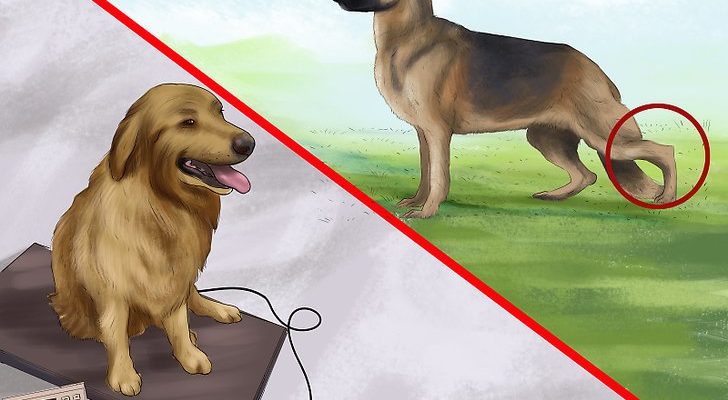
It’s painful to see your dog suffer from joint pain. These signs and treatments of hip dysplasia in dogs - inspired by The Parable of the German Shepherd - will help you recognize and treat your dog’s joint pain.
Blog Posts
Here's how to decide what to do when you’re confused, scared, or anxious. When you don't know what to do, you need inspiration from the Warrior and the Pineberries.
In this job description of log home builders, an experienced builder shares tips for working in the construction business. Learn what it's like spend your days in construction.
This list of classic board games for adults includes a brief history of each game and what makes the board games classic. These "gifts for gamers" also includes links,so you can get more information.
Whether you're in the dog walking business or hiring a dog walker, you'll want to know the rates I pay for my two dogs in Vancouver – and they may tempt you to start a dog walking business!
These gift ideas for a friend going through a divorce range from towers of happiness to tools of empowerment, and will help your friend see divorce as a beginning - not just an ending.
If you know how to produce positive energy, you will attract good things in life! These four law of attraction tips are based on The Secret, whichs holds that you send out negative and positive energy constantly. And, you attract what you emit. How, then, do you make sure you produce positive energy so you attract good things into your life? I have some ideas for you…but before we dive into my four tips for producing positive energy, check out this quip from Dr Joe Vitale: “Everything …
The most successful bloggers always ask, "What is a good blog?" Here's a summary of the best tips from professional bloggers and Google gurus, to show you what a good blog is.
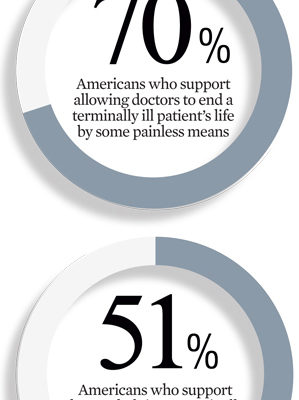
Here are three ways to describe what “death with dignity” is for people at the end of their lives – as well as for caregivers who love them, work with them, and support them in different ways.
Here's a list of jobs for introverts and quiet people, plus job search tips for introverted personality types. If you're an introvert, you're in the minority! But that doesn't mean it's "bad" to be an introvert...
A funeral director’s job involves helping people plan funeral services with compassion and empathy. In this career profile, a funeral director describes the challenges and rewards of working in a funeral home, and offers career tips for people interested in this caring profession. Sherry Varkel, an Ontario licensed funeral director since 1997, says that people are often surprised by the personalities of people in her field. “We all have good and positive attitudes,” she says. They need to in order …
Owning a costume rental shop is fun in many ways – and hard work in others! In this job description, a costume rental store owner describe the ups and downs of owning and managing a fancy dress shop. Most customers are surprised that you can get such a huge assortment of costumes in a rental shop – they can come in looking one way and walk out looking like Freddy Mercury, Shrek or Marilyn Monroe! For some customers, …
These five simple do-it-yourself dog massage techniques are from certified canine bodywork practitioners. I interviewed them for an article on pet massage I wrote last year for alive magazine in Vancouver.
In this interview, author Kerri Krysko describes writing the first Hells Angels book, a self-published memoir about being a Hells Angels ex-wife, called Kerri On: A Memoir of a Hells Angels Ex-Wife.
How are other people's expectations holding you back? These five tips for letting go of expectations are based on inspiration from Maria Shriver,